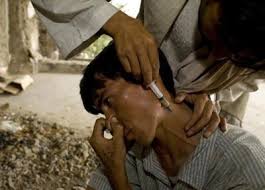
Brain changes effected by drug addiction

Brain changes effected by drug addiction. Curing the addicted brain from the effects of drug addiction
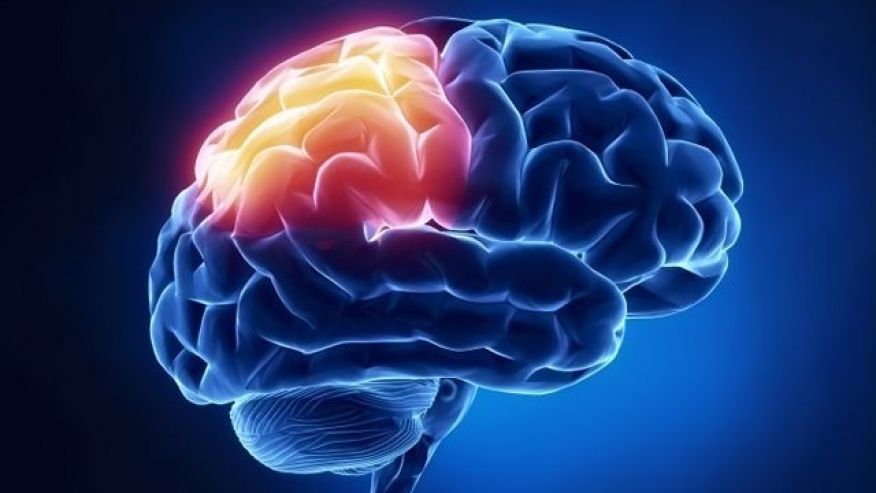
Brain changes effected by drug addiction: The prefrontal cortex
When the brain changes effected by drug addiction is wearing you down, there will always be some remedial actions to be taken. The prefrontal cortex will enables us to make rational, sound decisions. It also helps us to override impulsive urges. If acted upon, these impulses urges can cause us to act without thinking. This is usually not in our best interest. For instance, suppose I’ve had a bad day at work. I may have an impulsive urge to tell my boss exactly what I think of her. To act on this impulse is not in my best interest. Fortunately, my prefrontal cortex is functioning quite well. I still have my job!
Obviously, this ability to inhibit impulses is very helpful. It enables us to function well in society. It protects us from harm by allowing us to consider the consequences of our actions. However, when the pre-frontal cortex is not functioning correctly, the opposite occurs. Addiction causes changes to the prefrontal cortex. These changes account for two characteristics of addiction: impulsivity and compulsivity.
Impulsivity is the inclination to act upon sudden urges or desires without considering potential consequences. Sometimes people describe impulsivity as living in the present moment without regard to the future. On the other hand, compulsivity is a behavior that an individual feels driven to perform to relieve anxiety. Once a person performs the compulsive behavior, the anxiety goes away and restores comfort. Thus, the presence of these behavioral characteristics in addicted persons indicates that changes to the prefrontal cortex have occurred. Unfortunately, these changes also make the discontinuation of drug use more difficult.
When we talk of addiction changes brain structure and their functions, the message being delivered is that an addiction is a process that coordinates the transition from impulsive to compulsive behavior. Impulsivity occurs during the early stages of addiction. During this phase, people impulsively act on powerful urges to experience the pleasure of their addiction. Anxiety is not associated with the urges during these early stages. Instead, addiction reflects acting on impulsive desire to receive immediate pleasure from the drug or activity. People are not considering the future consequences.
Brain changes effected by drug addiction: The shifting progress of addiction
As addiction progresses a shift begins to occur. At this point, the compulsive aspect of addiction takes hold. When this shift occurs, people are no longer pursuing their addiction solely for pleasure. The compulsions compel them to participate in their addiction to relieve anxious, uncomfortable feelings. These may rise at the mere thought of stopping addiction for any reason (supply shortages, lack of opportunity, etc.). At this later compulsive stage, “pleasure” comes in the form of relief from these anxious, uncomfortable feelings. Thus, despite the negative consequences of addiction, the addictive behavior continues in a compulsive manner.
Finally although addiction damages the brain’s brakes (pre-frontal cortex) this is not to say there is a complete loss of control. We are not slaves to our biology. We have a tremendous amount of control over our actions. This is true even when impulsive and compulsive forces are operating. This recognition is vitally important if someone wishes to recover from addiction. When a person consciously decides the costs of addiction outweigh its benefits, they become motivated and able stop. This allows them to actively counter the effects of addiction on the frontal cortex and other brain regions. Therefore if this description suits your situation, then you are in the right path and calling doctor Akoury today will go a long way in helping you solve all the addiction problems you may be having.
Brain changes effected by drug addiction: The prefrontal cortex
http://www.awaremednetwork.com/